The overriding principle of all waste management is: don’t create it if you can avoid it. And if you must create the waste, seek ways to keep the quantity small and generation rate low.
Waste minimization is a buzzword, but it’s a buzzword that gives managers and operators a guiding tenet. Sometimes simple redesign can reduce waste quantities; other times attention to post-generation handling can reduce needless dilution or mixing of the waste.
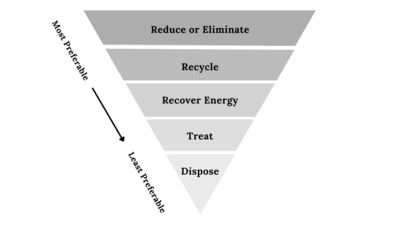 Waste management programs should concentrate on the facility operations, in particular those that generate the most waste. An educational program for employees can try to influence behavior - to keep employees mindful about waste production and segregated correctly so as to reduce the load on downstream treatment processes.
Waste management programs should concentrate on the facility operations, in particular those that generate the most waste. An educational program for employees can try to influence behavior - to keep employees mindful about waste production and segregated correctly so as to reduce the load on downstream treatment processes.
Healthcare managers can also reduce the production of waste through adapting their purchasing and stock control strategies.
Inventory control techniques can help reduce waste. For instance, more frequent ordering of small quantities rather than less frequent larger orders can result in lower levels of inventory, reducing the chances of product expiration. Using the oldest items in the inventory first, making sure to use all content of every container, and monitoring expiration dates can help reduce getting stuck with excess product.
While purchasing methodologies differ from organization to organization, if you are looking to reduce waste, you may wish to look to centralize purchasing. An inventory control system can help you use all the contents of every container and reduce losses to product expiration. Keeping track of chemical use throughout the facility can help reduce production of hazardous or infectious waste.
This is one of the general principles of chemical process design, and it applies more widely, even to mixtures of solid particles. It is related to the second law of thermodynamics. You can often theorethically separate materials, but only at the cost of energy. Sometimes that cost can be prohibitive.
This is one of the general principles of chemical process design, and it applies more widely, even to mixtures of solid particles. It is related to the second law of thermodynamics. You can often theoretically separate mixtures of materials, but only at the cost of energy. Often that cost can be prohibitive.
In waste management, we want to keep different types of waste separate unless there is a reason to combine them.
Don’t dilute your waste – unless you have a very good reason to do so. Dilution increases volume and disposal cost is usually directly proportional to volume or mass.
Don’t mix two different types of waste together – unless you have thought long and hard about it. By putting more than one type of physical or chemical waste in the same batch, you are increasing the specifications on the treatment or disposal system.
Keeping different types of waste in the same room or building is often OK. The safety measures for preventing release to the environment installed in a room may work for more than one kind of waste.
Accidental releases happen - spills, leaks, etc. Responsible waste management calls for measures to contain those releases. These include double-walled tanks (used for some hazardous materials, but rarely used in waste containment), sealants on concrete floors, berms around tanks, and measures to direct air flows inside buildings.
Some facilities with highly dangerous materials (e.g. nuclear facilities, laboratories that deal with virulent pathogens) use negative air pressure to reduce the chance of accidental release to the environment. Negative air pressure just means the pressure where the hazardous material is lower than in the surrounding area. The difference in pressure does not have to be great. Even a few inches of water pressure difference will cause air moving through minor leaks in the building to move from outside to inside. The air in the lowest pressure room is blown with fans through high efficiency filters to outdoors.
Good industrial hygiene practices should be followed where waste is treated or stored. This includes monitoring for known hazards in the air.
Regulators look at streams with more than one classification of waste in it and insist that management (storage and treatment and disposal) be appropriate for all types of waste. So a waste batch that included RCRA hazardous and pathological waste would have to satisfy regulations for hazardous waste and pathological waste before it is sent to disposal. The waste manager must keep this in mind, as mixtures of waste are often more expensive to treat.
This cost increase is more obvious when one thinks about mixing regulated waste (RCRA hazardous or radioactive or biohazardous) with harmless healthcare general waste waste (e.g. paper from administrative activities). The resulting increase in mass and volume needlessly raises treatment and disposal costs.
Best management practices are operating practices/procedures that minimize emissions. Often these are practices where employees or plant personal are trained to do something in a specific way every time they do the activity to reduce emissions. So, for instance when a barrel is used to drain equipment (doing MSS) the employees would be trained to immediately put a lid on the barrel once the draining has stopped. They don’t walk off for a coffee break or check their phone or do anything else until that lid is on.
 The ancient Greeks put medical instruments in boiling water to clean them. Even without the germ theory they knew from observation that heat tended to reduce the transmission of disease. Heat is used in treatment of infectious and other medical waste in many ways.
The ancient Greeks put medical instruments in boiling water to clean them. Even without the germ theory they knew from observation that heat tended to reduce the transmission of disease. Heat is used in treatment of infectious and other medical waste in many ways.
Boiling water is limited in temperature to 212 °F or 100 °C in an unpressurized container. (In a pressure vessel the boiling point can rise.) While this is hot enough to kill or deactivate most pathogens, a higher temperature is required to ensure the most hardy bacterial spores are eliminated. Autoclaves typically operate at 240 °F. Incineration takes place at temperatures above 1000 °F (and often 1800 °F or more) which is far above the temperature required to kill organisms and denature viruses.
Low-heat thermal processes find their way into many cleaning processes. Steam cleaning of room floors and walls is used to both clean (remove dirt) and disinfect. Microwave treatment is a low temperature thermal process.
The closer (in both space and time) you address the waste, the better. By address, we mean treat or package for final disposal. This principle is a guide for planning and process design. It can be violated if the overall big picture considerations call for it. One violation is the shift in medical waste incineration from locations close to point of generaion (hospitals) to larger facilities where waste from many hospitals is processes. The shift means waste must now be transported to the incinerator.
When the risk is uncertain it must be regarded as significant and protective measures must be taken accordingly.
"Better safe than sorry." The precautionary principle has been around for centuries and has informed safety considerations in engineering design. Some people divide it into a strong and weak precautionary principle. The strong principle, roughly, does not consider costs. This principle is most valuable in dealing with complex systems.
In the words of Shane Parrish: "When handling risks, it is important to be aware of what we don’t or can’t know for sure. The Precautionary Principle is not intended to be a stifling justification for banning things—it’s a tool for handling particular kinds of uncertainty. Heuristics can guide us in making important decisions, but we still need to be flexible and treat each case as unique."
One form of the strong principle is The Wingspread consensus statement was developed at a 1998 conference in Wisconsin about public health and waste:
When an activity raises threats of harm to human health or the environment, precautionary measures should be taken even if some cause and effect relationships are not fully established scientifically. In this context the proponent of an activity, rather than the public, should bear the burden of proof.
You're never going to have a zero waste facility. This is more or less a consequence of the second law of thermodynamics. You can't practically recycle everything or stop all waste production. Zero waste is fine as a bright shiny object, but realize you will never get there. The best you can do is to asymptotically approach it.
Medical waste is any waste produced at a medical facility, but most of that waste is not different from waste produced at a law firm or retail store. It is not specially hazardous or contaminated with biological material. It is much easier to deal with than the other types of medical waste we discuss on this website. The only thing to remember is: keep this waste from mixing with the more serious hazardous, radioactive, sharps, or biomedical waste.
In the United States we call this general waste Municipal Solid Waste. It is ubiquitous. Your household produces it. The corner store produces it. The office produces it. It is in a sense a solved problem in the sense that we don’t think about it much any more. Maybe we shouldn’t as the waste still exists, we just put it in a landfill.
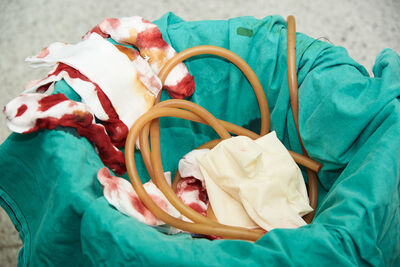 Regular non-hazardous municipal solid waste is cheap to store and dispose of. At-risk medical waste (infectious, pathological, hazardous, radioactive, or regulated) is much more expensive. How much more expensive? There is no general answer for that and both relative and absolute costs depend on geography, market supply and demand, and alternatives. A rule of thumb for budget estimates is that these waste cost ten times as much to dispose of as general non-hazardous waste. If you are an ambitious waste management professional, you might want to try to calculate how much each of your waste streams costs to store and dispose of on a per pound basis.
Regular non-hazardous municipal solid waste is cheap to store and dispose of. At-risk medical waste (infectious, pathological, hazardous, radioactive, or regulated) is much more expensive. How much more expensive? There is no general answer for that and both relative and absolute costs depend on geography, market supply and demand, and alternatives. A rule of thumb for budget estimates is that these waste cost ten times as much to dispose of as general non-hazardous waste. If you are an ambitious waste management professional, you might want to try to calculate how much each of your waste streams costs to store and dispose of on a per pound basis.
What do I do with Medical Waste?
