The primary methods of treating medical waste are:
In the past, medical waste produced at hospitals was primarily treated on-site. Over time, the expense and regulation of treatment have prompted clinics and medical facilities to hire contractors to haul away their waste for treatment and disposal off-site, and the percentage of medical organizations that perform their own treatment and disposal has dropped.
Incineration is the controlled burning of the medical waste in a dedicated incinerator. Among industry professionals, these units are often referred to as hospital/medical/infectious waste incinerators (HMIWIs).
Incineration is an old technology and was widely used in the past for all sorts of waste. Individual buildings had their own waste incinerators in many cases. Incinerators got a bad reputation because of the air pollution they created and because the bottom ash, or clinker, was hard to keep under control. Members of the public unfortunately still have negative associations with incinerators. Today’s incineration units are typically much cleaner.
There are parts of the world where open pit burning still takes place. And accidental fires - e.g. burning houses - produce flames and smoke and debris. This makes “burning” and “combustion” unsavory words, but when approached from a cold hard engineering standpoint, incineration is often the best technology for treating medical waste. It eliminates pathogens - even hard-to-kill bacterial spores - and can reduce the volume and mass of waste that goes to landfills by 80 percent or more. Incineration can break down and render harmless hazardous organic chemicals. With proper technology, little acid gas is released to the atmosphere.
Engineers often look at expected heat generated by combustion when choosing which incinerator to use: waste with heating value over 3500 kcal/kg is processed in a pyrolysis unit while lower heating value waste is burned in a single-chamber incinerator. (For reference, dry wood has a heating value of about 3800 kcal/kg and charcoal has a heating value of 7000 kcal/kg. ) Waste is typically heterogeneous, and if the combustible fraction is below 60 percent, it may not be acceptable for incineration. Overly wet waste (over 30 percent water by weight) is probably not good for incineration either as it will require excessive quantities of assist gas/fuel.
Incineration requires no pretreatment. The resulting solid ash can be disposed of in traditional methods, such as landfilling. Secondary waste from the air pollution control system (scrubber waste) may be classified as hazardous under RCRA. Modern incinerators can provide a secondary benefit by creating heat to power boilers in the facility.
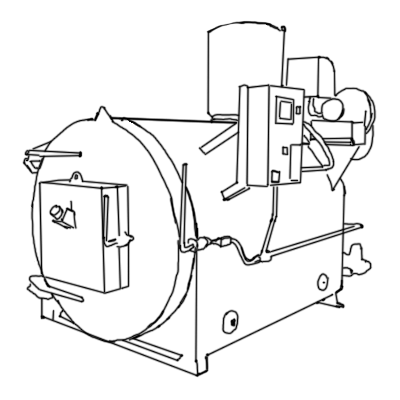
The public often has an aversion to incinerators and may raise objections if they hear one is being put in their area. The popular perception of incineration is informed by pictures of open pit burning done decades ago in the US and still today in some countries. Open pit burning is indeed not effective enough and results in smoke and other undesirable materials being released to the atmosphere. Most people don’t understand how incineration units can be made clean-burning and engineered to reduce the risk of dangerous releases. Most people also don’t understand how many incinerators are in their area already.
However, incineration can be a dirty process if not controlled adequately or if the process has not been designed correctly. Incineration can produce:
Even small incinerators can be optimized with good engineering design and operating procedures. The size and the throughput should be balanced to ensure a high residence time in the furnace. A good rule of thumb is to aim for 1200 °C with a vapor-phase residence time of 2 seconds.
Operation of medical waste incinerators.
Mechanical treatment does not kill pathogens or disinfect equipment, but it can reduce waste volume and increase the surface area in preparation of further treatment or disposal. Crushers and milling machines break down solid pieces of waste. Mechanical shattering or splintering of waste can also alter its appearance, which can be useful in lessening the psychological impact of the waste on human observers. More on shredders.
Autoclave treatment of medical waste.
Other methods of waste treatment.
Integrated treatment systems for medical waste.